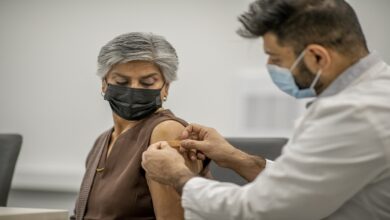
How BRCA Status Impacts Ovarian Cancer

Rozzie* has a thing for teal nail polish. “I wear teal nail polish all the time—summer teal and winter teal,” she says. It’s more than a favorite color: This specific blue-green shade signifies awareness and support for the more than 21,410 American women› who will receive a diagnosis of ovarian cancer this year. Rozzie learned she had the condition in 2012.
“People will comment on my nails, and I’ll respond with ovarian cancer facts,” Rozzie says. “I carry the signs and symptoms handout in my purse with me and share it with people that I talk to in my everyday life. In that way, I can reach one person at a time, and that’s one more person who knows and can spread the word.”
After Rozzie was diagnosed with ovarian cancer, she explained her family history of cancer to her doctor, who then recommended she undergo genetic testing. Genetic testing identifies inherited mutations which can inform family risk for certain cancers, or eligibility for treatment options once diagnosed with certain cancers. The results determined that she had a harmful BRCA mutation that had dramatically increased her cancer risk.
Understanding BRCA mutations
BRCA1 and BRCA2 are human genes that produce tumor-suppressing proteins, according to the National Cancer Institute (NCI). These proteins help repair damaged DNA but, when either gene is mutated or altered, DNA damage may not be repaired. As a result, the cells with unrepaired DNA are more likely to develop genetic alterations that can lead to cancer. The risk for certain types of cancers varies between BRCA1 and BRCA2. For example, those with a BRCA1 mutation are more likely to get ovarian cancer than those with a BRCA2 mutation according to a study of 5,066 women.
BRCA gene mutations can be passed through families. Several cancers, including breast, ovarian, fallopian tube, peritoneal (abdominal cavity), prostate, and pancreatic, have been linked to harmful BRCA gene mutations. Because BRCA mutations can be hereditary, they can be passed down to family members regardless of gender. For example, they could be passed from a father to his daughter or son, or a mother to her son or daughter. These mutations can sometimes explain why cancer seems to “run in the family” for some people. It has for Rozzie.
“My mother was 47 when she died from colon cancer, and her brother died of the same disease,” Rozzie says. “My father died of prostate cancer, and my father’s sister died from pancreatic cancer,” she says. “Cancer was present in both sides of my family, but I do not know which side of the family I inherited the gene mutation from.”
Knowledge is power
Armed with the knowledge of her inherited BRCA status, Rozzie’s doctors were able to pinpoint her best course of treatment. These findings also prompted Rozzie’s daughter, Ilana,* to undergo genetic testing. She learned that she also had an inherited BRCA gene mutation that increased her cancer risk and opted to have a preventative oophorectomy, a surgery where one or both ovaries are removed to minimize the risk of developing cancer. And she is so thankful she did. “When I woke up from surgery, I was told that I already had stage 2 ovarian cancer,” says Ilana.
Rozzie also has a son, Brian, who hasn’t undergone genetic testing yet, but plans to in the future. In the meantime, knowing he has a 50/50 chance of inheriting the BRCA gene alteration, he met with a genetic counselor so he would know what steps to take if he ever tests positive for the mutation or receives a cancer diagnosis. He also takes preventative measures including undergoing annual prostate cancer screenings and colonoscopies, and giving himself regular self-breast exams.
Now Rozzie is on a mission to increase awareness of ovarian cancer and how genetic testing might help people protect their health. “It’s my passion,” she says. “If I wasn’t diagnosed with cancer and been tested, the most precious life to me, my daughter, wouldn’t have been tested and might not be here today. Through genetic testing, I was able to save my daughter’s life. And I want every parent to be able to do that for their child.”
Genetic testing isn’t routinely discussed at annual gynecologist visits, and, understandably, you might have some questions about it, as well as how the whole thing works. Here is some of the most vital information you should know about determining your BRCA status, understanding how it relates to your ovarian cancer risk, and how your BRCA mutation status can inform your treatment options if you develop cancer.
Having the BRCA gene mutation increases your ovarian cancer risk.
About 1 in 300 people to 1 in 800 people are estimated to carry an inherited BRCA1 or BRCA2 mutation, according to the American College of Obstetricians and Gynecologists (ACOG). About 1.3% of women in the general population will develop ovarian cancer during their lifetime. But 44% of women who inherit the harmful BRCA1 mutation and about 17% of women who inherit the harmful BRCA2 mutation will develop ovarian cancer by the age of 80, the NCI says.
If you discover that you have a BRCA mutation, your doctor will want to discuss next steps to lower your cancer risk. Options range from frequent screenings to prophylactic surgery (a procedure intended to prevent disease), per the NCI. This type of surgery, like the oophorectomy Ilana chose to undergo, is a personal decision that should be discussed with your family and doctor.
Genetic testing is recommended for at-risk women 25 and older.
“In general, genetic testing for BRCA1 and BRCA2 is not recommended until age 25, as this is when cancer prevention interventions, like breast MRI for breast cancer screening, start,” says June Y. Hou, M.D., co-director of the Hereditary Breast and Ovarian Cancer Program at Columbia University Medical Center and NewYork-Presbyterian Hospital. “Ovarian cancer screening typically does not begin until age 30.”
There are exceptions, though. Dr. Hou says, “particularly if there is a diagnosis of a BRCA1 or BRCA2-related cancer at a very early age.” So, it’s important to talk to your doctor or a genetic counselor about your individual risk.
If you have a BRCA mutation, you might need more frequent screening or surgery.
If you test positive for an inherited BRCA gene mutation, you’ll typically meet with a genetic counselor or doctor to discuss the types of cancers you’re at an increased risk for and what the results mean for you and your family members, says Christine Steele, a certified genetic counselor at Moffitt Cancer Center. “There are management guidelines—including things like more frequent screenings or surgery—that can be put in place to improve the likelihood that cancer is detected at an early and treatable stage or prevented,” she says.
Remember, testing positive for a harmful BRCA mutation doesn’t mean you’ll get cancer.
While both Rozzie and Ilana tested positive for a harmful inherited BRCA gene mutation and were diagnosed with cancer, Steele says that you shouldn’t panic if you test positive.
“[Testing positive for a] BRCA gene mutation means that someone is at a higher risk of developing certain cancers—it does not mean they are certain to develop cancer,” she says. “Because we know carrying a BRCA gene mutation puts people at a higher than average risk of getting cancer, we can personalize their screening and prevention regimen to keep them as healthy as possible.”
However, if you do get cancer, knowing your BRCA status can help your doctors choose the best treatment plan.
Knowing your BRCA status will help your care team decide what treatment options are best for you, the NCI says. For instance, if you are diagnosed with ovarian cancer and have a BRCA1 or BRCA2 mutation, a PARP inhibitor might be helpful. This class of targeted therapy promotes cancer cells not to repair their damaged DNA, causing them to die, according to the NCI.
Ultimately, knowing your BRCA gene status can empower you to make better choices about your health. To learn more about testing for your BRCA gene status, check out beBRCAware. There, you can learn more about testing options, how to find a genetic counselor, and next steps.
*Rozzie’s, Brian’s and Ilana’s last names have been withheld to protect their privacy.
This content is created and maintained by a third party, and imported onto this page to help users provide their email addresses. You may be able to find more information about this and similar content at piano.io
Source link