California coronavirus variant may spread faster, inflict severe disease, early data suggests
[ad_1]
Early data suggests a coronavirus variant first detected in California may be more transmissible, possibly cause more severe disease, and could have an impact on vaccine efficacy.
Study authors are awaiting approval from public health departments for publishing of a preprint, though Dr. Charles Chiu, co-study author and professor of laboratory medicine with the University of California San Francisco, shared and elaborated on the findings to Fox News.
“I am worried, concerned but not panicking about this,” Chiu said. “This is something that needs to be further investigated and I really think that at this point we don’t know enough to recommend any changes to the standard public health measures that we use to prevent infection.”
JOHNSON & JOHNSON COVID-19 VACCINE HAS ‘FAVORABLE SAFETY PROFILE,’ FDA STAFF FINDS
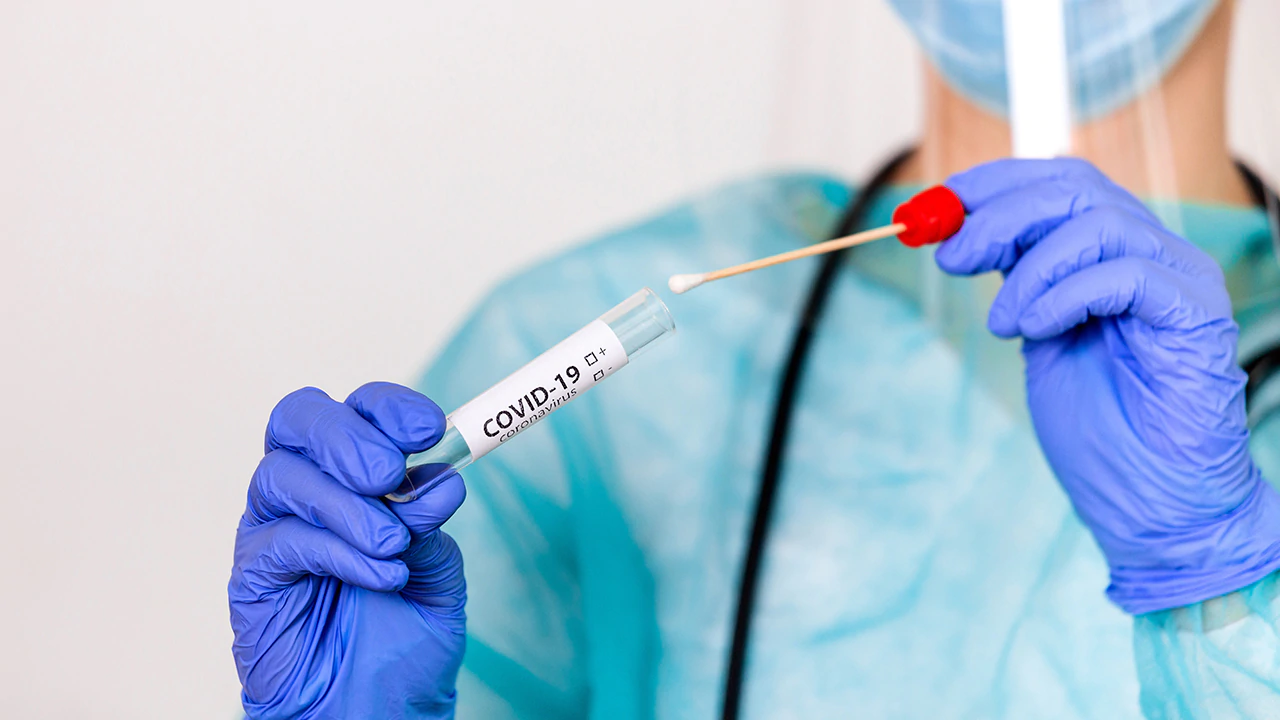
The team sequenced viral genomes from 2,172 nasal samples from COVID-19 patients across 44 counties in California from Sept. 1, 2020 to Jan. 29, though sequencing was concentrated in major metropolitan areas like Los Angeles, Alameda, San Francisco and Santa Clara counties.

The team analyzed nasal swabs from over 2,000 genomes to gather findings.
(iStock)
The variant, dubbed B.1.427/B.1.429 or 20C/L452R, swelled to account for over 50% of cases across multiple counties over the five-month sampling period. The study notes the variant was detected in 459 of the 2,172 sampled genomes, or about 21%. The first reported case of the variant occurred in July in Los Angeles, though sequence analysis suggests it likely emerged in May 2020. This variant includes a key unique mutation dubbed L452R not seen on other concerning variants like those first identified in the U.K. Brazil and South Africa, among other mutations.
“We managed to obtain some evidence that this is a more infectious variant,” Chiu said, noting a two-fold increase in patients’ virus concentrations in the nasal swabs. “That doesn’t necessarily prove, but does suggest, that it may be more infectious.”
JOHNSON & JOHNSON COVID-19 VACCINE READY FOR ROLLOUT ‘WITHOUT DELAY’ PENDING EUA, WHITE HOUSE SAYS
Another line of evidence behind increased transmissibility involved pseudoviruses that researchers genetically engineered to include the key L452R mutation.
“We found out that those viruses were at least 40% more infectious than viruses that did not have that mutation,” Chiu continued. “The key mutation that’s found in this variant appears at least in vitro, in the lab, to be more infectious to cells.”

Public health experts say the same mitigation measures, like mask use, proper distancing, hand hygiene and prompt, widespread vaccination will help protect against variant strains of the virus.
(iStock)
Three lines of evidence combine to form clinical, laboratory and other data backing claims that the variant could be more tranmissible.
What’s more, when researchers examined 13 blood samples from recovered patients and vaccine recipients, and tested how well the antibodies neutralized the variant compared to other strains, the antibodies in the blood from two of three recovered patients were four-fold less effective in neutralizing the variant, and antibodies from six of eight vaccine recipients were two-fold less effective in neutralizing the variant.
Chiu said these vaccine recipients received two doses of either the Pfizer or Moderna vaccines.
MICHIGAN BOY WITH RARE CORONAVIRUS-RELATED INFLAMMATORY ILLNESS ENDURES 4 AMPUTATIONS
Studies have suggested the South African variant dropped the Pfizer vaccine’s neutralization power by about two-thirds, while Moderna saw a six-fold reduction in neutralizing antibodies. Chiu notes that the California strain, by way of comparison, lent a “moderate” effect.
The coronavirus variant lent a “moderate” reduction in neutralizing power from the recently-approved vaccines, study authors said.
(iStock)
The retrospective analysis assessing for virulence, or severe disease associated with the strain, was a difficult analysis, but findings from 324 hospitalized COVID-19 patients at a tertiary hospital suggested an increased association with ICU stay and death. More specifically, the variant was detected among 69 patients. Chiu said 11% of hospitalized patients infected with the variant died, compared to 2% of hospitalized COVID-19 patients infected with a different strain. This difference is statistically significant, he said.
“As the number and proportion of severe cases were low in our cohort, resulting in wide confidence intervals, further investigation is needed to confirm these findings,” the study reads. “In addition, as shown for B.1.1.7, it is difficult to discriminate between whether the variant is inherently more virulent or whether the higher risk of severe disease is related to other factors such as increased transmissibility resulting [in] an influx of cases that can strain available health care resources.”
“This is still very preliminary data, but it does suggest that there may a potential association between more severe disease from infection from the variant,” Chiu said.
There are still unanswered questions, like the exact mechanism behind the key L452R mutation. While the mutation is located in the same region (the receptor binding domain) as other mutations identified in global variants of concern, it doesn’t come into direct contact with the ACE2 receptor, compared to the N501Y mutation on the B.1.1.7 variant first detected in the U.K., for instance. Instead, the mutation comes into close proximity with the ACE2 receptor, and separate early data suggests the mutation helps to stabilize the interaction between the spike protein and the ACE2 receptor.
Chiu said it’s unclear at this point whether the strain is responsible for a sharp increase in virus cases in California. State data shows California experienced a severe surge in cases from late December to mid-January, logging over 40,000 daily infections. Chiu said a so-called “genetic drift,” or a random emergence of the “right strain at the right time” could also be behind the surge. Another puzzling piece is the timing behind the state’s case surge, when the variant likely emerged earlier last spring. Researchers are still working to answer this question.
The key L452R mutation has also previously been found in Denmark, but this was not the same variant, which hosts its own set of unique mutations.
CLICK HERE FOR COMPLETE CORONAVIRUS COVERAGE
The California variant has yet to arise to the level of a “VOC,” or variant of concern, likely because of the unknowns associated with it so far, the study author said. This decision to coin the strain a “VOC” should ultimately be left to public health authorities and the Centers for Disease Control and Prevention, Chiu said.
Chiu said researchers “urgently” need to accumulate more data to further confirm the findings, especially initial findings regarding infectivity, transmissibility and effect on neutralizing antibodies.
[ad_2]
Source link






