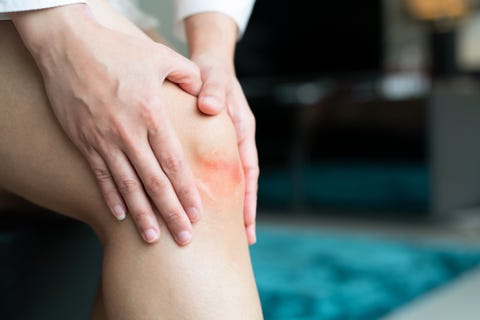
How To Spot The Difference Between Chronic and Acute Inflammation

The “I” word is a biggie in the health world: inflammation. And it has somewhat of a split personality. Inflammation occurs naturally in the body and plays a key role in helping you recover from injury, trauma, and even a simple cut. That’s good. But it’s also at the root of a whole slew of serious health conditions and diseases. Not so good. On one hand, inflammation can help you heal, and on the other, it can make you sick.
Types of Inflammation
There are two main forms of inflammation: acute and chronic. Acute inflammation is how your body helps you heal short-term from something like an infection (you get a cold and don’t feel great for a week while your body works to rehab itself) or trauma (you bumped your knee and it swells as your body goes into repair mode). Most of the time, this inflammation is positive. Chronic inflammation happens when inflammation builds up inside your body and hangs around longer than it needs to (from stress, diet, or disease, for example)—and that can have negative effects on your health. Research suggests that chronic inflammation plays a role in everything from heart disease and arthritis to diabetes and cancer.
And just to complicate things, acute inflammation isn’t always benign. In the case of acute joint pain, for example, there’s a risk of infection or trauma, meaning that sometimes acute inflammation can be just as problematic as the chronic kind.
Phew. All of this brings us here: It’s important to be able to identify between the two different types of inflammation, but it’s also important to know when you might need to consult a doctor. Here’s how to figure out what type of inflammation you’re dealing with and what to do about it.
If your inflammation is widespread: It might be chronic
Generally speaking, systemic inflammation—inflammation that impacts a lot of different parts of your body—points to a chronic health issue, says Julie Chen, M.D., a nationally recognized integrative medicine doctor based in San Jose, CA. If you have chronic inflammation, you might describe your pain as more of an “all over” feeling or just generally feel pain in a lot of different places. Symptoms such as fatigue and achiness can be signs of chronic inflammation.
What to do: Depending on your symptoms, talk to your doctor about what kind of tests they may be able to do. Different blood tests or other diagnostic tests can measure biomarkers of inflammation that give clues into what could be going on. There are also many lifestyle interventions that can help you feel better. Take weight loss: Research shows that in people with psoriatic arthritis, a type of arthritis caused by chronic inflammation, weight loss on its own can significantly improve people’s disease and lower their levels of inflammation. If your symptoms are getting in the way of your day-to-day, talk to your doctor.
If your inflammation seems to be in one spot: It’s probably acute—but it depends
Localized swelling and pain—say, around your shoulder or your knee—could be acute inflammation. But chronic inflammation can sometimes show up in one area, too (and stick around for weeks or months). “For many chronic inflammatory skin diseases, inflammation tends to occur in the same locations,” says dermatologist April Armstrong, M.D., chair of the National Psoriasis Foundation Medical Board, and associate dean for clinical research at Keck School of Medicine at University of Southern California. To figure it out, your doctor may ask questions about how long the pain has been lingering.
What to do: That depends; don’t write off localized inflammation (say, a swollen wrist or puffy feet) just because it’s in one spot. Always seek out medical attention if you’re in pain or worried about it, since acute joint pain can require a medical professional to check for infection or trauma, says Anca D. Askanase, M.D., M.P.H., a professor of medicine in the division of rheumatology at Columbia University College of Physicians & Surgeons.
Otherwise, noting how long a rash has been at a certain location, for example, can shed light on acute versus chronic inflammation, and help you decide whether to get it checked out.
If your inflammation has been around 6+weeks: It’s probably chronic
Whether you’re talking about your skin, your joints, or both, keeping track of how long you’ve had symptoms is a good idea. Chronic inflammation of the skin can last for months or even years, explains Dr. Armstrong, while acute inflammation typically clears up in a few days or weeks. As for your joints? “Chronic inflammation in the joints lasts longer than six weeks and defines chronic arthritis,” says Dr. Askanase.
What to do: There’s no need to wait a certain amount of time before you seek help; you should always see your doctor if you’re in pain, says Dr. Chen. And if pain and inflammation have been present for longer than six weeks, you definitely need to book an appointment with your health professional STAT.
If over-the-counter (OTC) or at-home remedies help you feel better: It depends
The majority of acute joint pain responds to traditional measures of rest, ice, elevation, and OTC anti-inflammatory drugs (think: ibuprofen). But that doesn’t automatically mean that inflammation tamed by more conservative measures is acute. Pain from mild, chronic inflammation can respond to OTC medications just as easily as acute inflammation can, points out Dr. Chen. Alternatively? “If acute inflammation is severe, then these medications won’t help, but that doesn’t mean that your pain is chronic,” she says.
What to do: Monitor your pain and keep an eye on whether it returns, and how long it lasts. But regardless of duration, if you’re in serious pain or have symptoms such as a fever (a potential sign of infection), always check in with your doctor.
If you can’t stop itching your skin and now it looks thick and leathery: It’s could be chronic
Notice raised areas of inflamed skin or scales or wrinkles that have built up on top the skin? That could be pointing toward a skin condition caused by chronic inflammation, explains Dr. Armstrong. “Sometimes the body’s natural response to chronic inflammation in an area is to grow thicker skin.” Doctors use the term ‘lichenification’ to describe the bark-like appearance of this skin. You don’t usually see this kind of a reaction with acute inflammation, which tends to be more short-lived, says Dr. Armstrong.
What to do: Make an appointment with a dermatologist or a rheumatologist, who can help you identify what might be going on. And do your best to not scratch at the area in the meantime.
This content is created and maintained by a third party, and imported onto this page to help users provide their email addresses. You may be able to find more information about this and similar content at piano.io
Source link